Advanced Carbon-Ion Radiotherapy
Overview
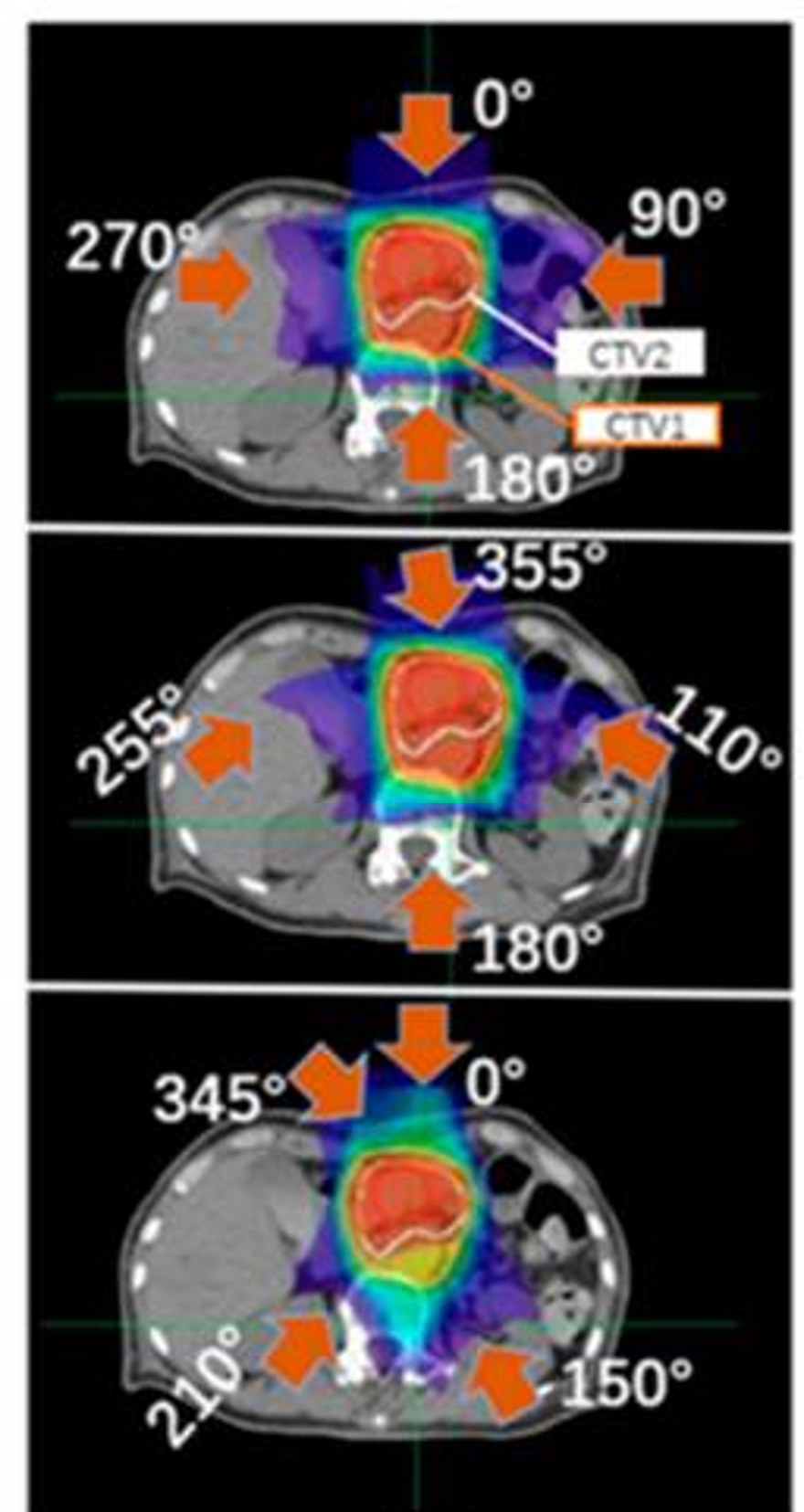
Carbon-ion radiotherapy is one of the most advanced forms of radiation therapy, in which carbon nuclei are accelerated to near the speed of light and used for cancer treatment. Compared with conventional photon (X-ray) radiotherapy, carbon-ion beams provide superior dose concentration to the target volume, enabling effective tumor control while reducing radiation exposure to surrounding healthy tissues. In addition, the high linear energy transfer (LET) of carbon ions leads to enhanced biological effectiveness, making this modality particularly effective for radioresistant tumors. However, precise alignment between the high-dose region and the tumor position requires sophisticated technologies and accurate dose calculations. Furthermore, patient conditions and internal anatomical structures can vary slightly from day to day, making adaptive strategies essential. Our research focuses on developing advanced irradiation and treatment planning methods to achieve more accurate and reliable carbon-ion radiotherapy.
Key Points
- High-precision dose calculation
- Treatment planning optimization
- Research design with an emphasis on clinical implementation
Selected Publications
Soft Errors in Medical Devices
Overview
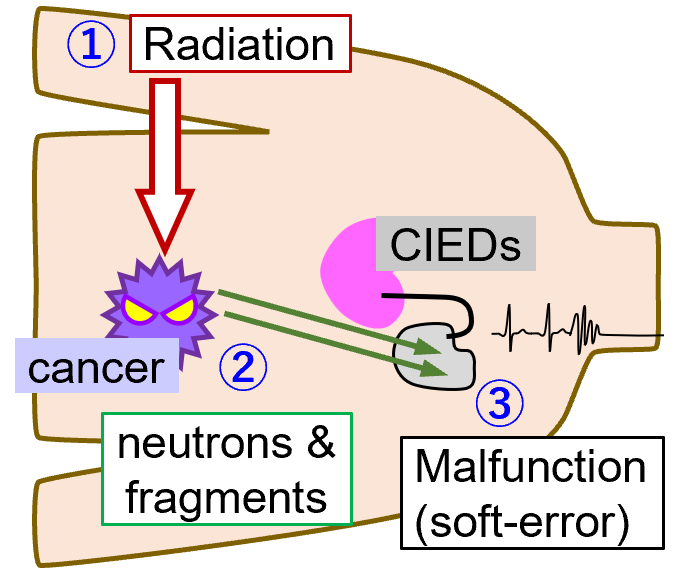
Radiation therapy is a minimally invasive cancer treatment modality, and its clinical applications continue to expand. However, in particle therapy and high-energy photon radiotherapy, secondary neutrons are generated during irradiation. When these neutrons interact with electronic devices, they can induce malfunctions known as soft errors. Such events are particularly critical for implantable cardiac electrical devices (CIEDs), including pacemakers, where malfunctions may pose serious risks to patients. To address this issue, we develop soft-error measurement systems that can be used inside treatment rooms, and evaluate the associated risks in clinical radiation therapy environments. In carbon-ion radiotherapy, not only neutrons but also various secondary fragment particles contribute to soft-error occurrences, and the risk strongly depends on irradiation conditions. As the number of patients requiring radiation therapy while using medical devices is expected to increase, our research aims to establish safer treatment strategies through quantitative risk assessment and mitigation techniques.
Key Points
- Neutron transport simulations using 3D treatment device models and patient CT data
- Measurement of high-energy neutrons
- Development of soft-error measurement systems
Selected Publications
Development of Medical Compton Cameras
Overview
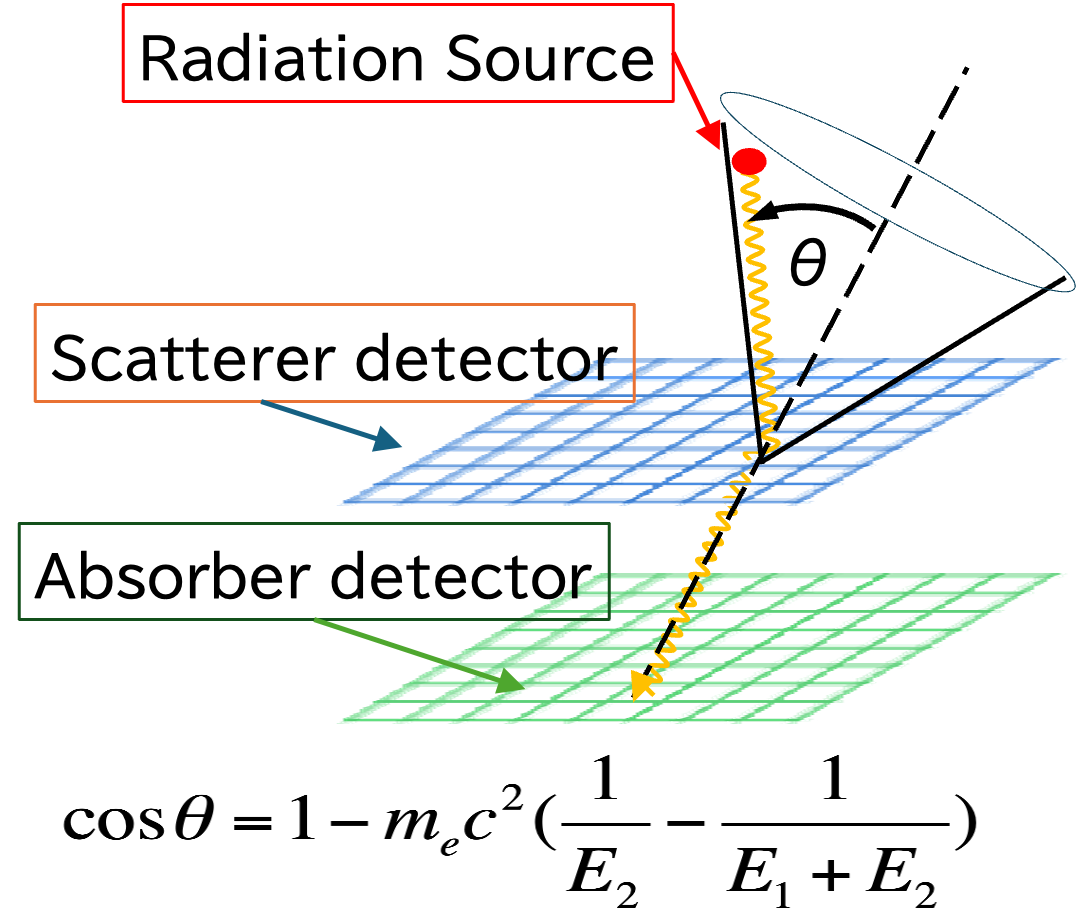
A Compton camera consists of two types of detectors, commonly referred to as a scatterer and an absorber. By combining the interaction position and absorbed energy information obtained from these detectors, the incident direction of gamma rays can be reconstructed based on the Compton scattering angle. Conventional gamma-ray imaging systems, such as pinhole cameras and SPECT, rely on heavy collimators to define the incident direction of radiation. However, for high-energy gamma rays or environments with strong background radiation, thick and heavy collimators are required, resulting in large and cumbersome systems. This makes such systems unsuitable for use in radiation therapy rooms, where space and portability are critical. Compton cameras do not require massive collimators, enabling compact and lightweight designs. Our research explores the application of Compton cameras to range verification in particle therapy and dose monitoring in boron neutron capture therapy (BNCT).
Key Points
- Machine-learning-based event selection and noise reduction
- Development of image reconstruction algorithms
- Evaluation of imaging performance